A case of spontaneous subarachnoid hemorrhage and intraventricular hemorrhage with negative computed tomography angiography findings
Introduction
The prevalence of cerebral aneurysms in the general population is approximately 2–3% (1-3) and small ruptured aneurysms <5 mm were found in about 40% of all spontaneous subarachnoid hemorrhage (SAH) patients (4). Although literatures (3,5) demonstrated that small cerebral aneurysms have a low risk of rupture, many experienced neurosurgeons and endovascular therapists report that most ruptured aneurysms encountered in practice are small (6,7). As seen in a study by Gupta et al., aneurysms smaller than 2 mm can also result in an SAH and constituted 7% of ruptured aneurysms (8). We hereby present a mid-aged female patient diagnosed with SAH and intraventricular hemorrhage (IVH) with negative findings on brain computed tomography angiography (CTA), which derived from a tiny cerebral aneurysm. The only clues at the first beginning were stiffness of neck and xanthochromia of cerebrospinal fluid (CSF). This was a rare case based on our experiences without efficient data on the best diagnostic strategies and emphasized the importance of clinical examination but imaging examination.
Case presentation
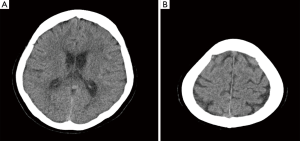
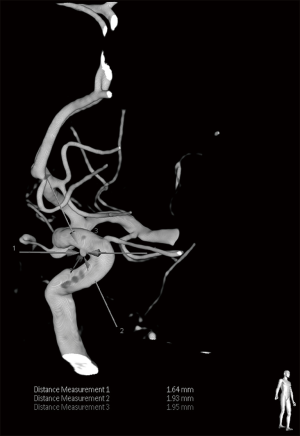
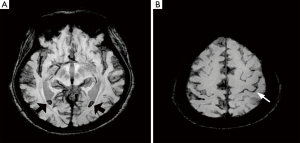
A 53-year-old woman was brought to the emergency department with sudden onset of explosive headache lasting more than 12 h. She had a past medical history of hypertension but didn’t take any medication regularly. There was no history of trauma, fever, swallowing problem and vomiting occurred. On neurologic examination, stiff neck and both of the Brudzinski’s sign and Kernig’s sign were noted, but the laboratory and physical examination were otherwise unremarkable. Brain CT (Figure 1) and CTA showed no abnormality. Lumbar puncture was performed, which demonstrated opening pressure 85 mmH2O and closing pressure 70 mmH2O and revealed turbid and pink CSF fluid on visual inspection. Her CSF analysis demonstrated 127 white blood cells per mm3 and >10,000 red blood cells per mm3, and xanthochromia by spectrophotometry in Figure 2. Because of SAH was highly suspected by the clinical history and presentation, digital subtraction angiography (DSA) was performed and showed a small saccular cerebral aneurysm (<2 mm) at ophthalmic segment of left internal carotid artery in Figure 3. Brain magnetic resonance imaging (MRI) also revealed SAH and IVH involving bilateral lateral ventricles in Figure 4. The patient received conservative treatment and discharged after an uneventful recovery. She has remained well at 6-month follow-up.

Discussion
About 80–85% of nontraumatic SAHs are caused by cerebral aneurysm rupture (2) and late diagnosis of this life-threatening disease will be dangerous. Meningeal signs and xanthochromia of CSF are the typical findings which is easy for physicians to check at the first beginning (9,10). Brain CTA is less invasive than DSA and more convenient for clinical management, but some smaller cerebral aneurysms are undetectable on brain CTA (2,11,12). A study performed by Wintermark et al. revealed that brain CTA only had a sensitivity of 50% for aneurysms <2 mm (12,13), though brain CTA has been reported a sensitivity of 97–100% for the detection of intracranial aneurysms in prior studies (9). DSA remains the gold standard for detecting and characterizing intracranial aneurysms, which identifies a cause of SAH in 4–14% of patients with negative brain CTA images (14,15). DSA should be performed based on the clinical picture highly suggestive of SAH (1,2).
Although brain CTA could help us making diagnosis more easily, physicians should be alert to the possibility of SAH even if there was no positive finding on brain CTA. Cerebral aneurysms which are smaller than 2 mm are less reliably detected by brain CTA (15-17). Patients presenting to emergency department with a sudden explosive headache and positive meningeal signs should be treated with caution. It is recommended that DSA should be considered if there is a highly clinical suspicion of SAH.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/ht.2019.11.02). WHC serves as an Editor-in-Chief of Health Technology. The other authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Grasso G, Alafaci C, Macdonald RL. Management of aneurysmal subarachnoid hemorrhage: State of the art and future perspectives. Surg Neurol Int 2017;8:11. [Crossref] [PubMed]
- Yang ZL, Ni QQ, Schoepf UJ, et al. Small Intracranial Aneurysms: Diagnostic Accuracy of CT Angiography. Radiology 2017;285:941-52. [Crossref] [PubMed]
- Zanaty M, Daou B, Chalouhi N, et al. Evidence That a Subset of Aneurysms Less Than 7 mm Warrant Treatment. J Am Heart Assoc 2016;5. [PubMed]
- Choi JH, Park HS. The Incidence and Characteristics of Patients with Small Ruptured Aneurysms (<5 mm) in Subarachnoid Hemorrhage. J Korean Neurosurg Soc 2017;60:424-32. [Crossref] [PubMed]
- Wiebers DO, Whisnant JP, Huston J 3rd, et al. Unruptured intracranial aneurysms: natural history, clinical outcome, and risks of surgical and endovascular treatment. Lancet 2003;362:103-10. [Crossref] [PubMed]
- Weir B, Disney L, Karrison T. Sizes of ruptured and unruptured aneurysms in relation to their sites and the ages of patients. J Neurosurg 2002;96:64-70. [Crossref] [PubMed]
- Korja M, Lehto H, Juvela S. Lifelong rupture risk of intracranial aneurysms depends on risk factors: a prospective Finnish cohort study. Stroke 2014;45:1958-63. [Crossref] [PubMed]
- Gupta V, Chugh M, Jha AN, et al. Coil embolization of very small (2 mm or smaller) berry aneurysms: feasibility and technical issues. AJNR Am J Neuroradiol 2009;30:308-14. [Crossref] [PubMed]
- Heit JJ, Pastena GT, Nogueira RG, et al. Cerebral Angiography for Evaluation of Patients with CT Angiogram-Negative Subarachnoid Hemorrhage: An 11-Year Experience. AJNR Am J Neuroradiol 2016;37:297-304. [Crossref] [PubMed]
- Yap L, Dyde RA, Hodgson TJ, et al. Spontaneous subarachnoid hemorrhage and negative initial vascular imaging--should further investigation depend upon the pattern of hemorrhage on the presenting CT? Acta Neurochir (Wien) 2015;157:1477-84. [Crossref] [PubMed]
- Bechan RS, van Rooij SB, Sprengers ME, et al. CT angiography versus 3D rotational angiography in patients with subarachnoid hemorrhage. Neuroradiology 2015;57:1239-46. [Crossref] [PubMed]
- Moran CJ. Aneurysmal subarachnoid hemorrhage: DSA versus CT angiography--is the answer available? Radiology 2011;258:15-7. [Crossref] [PubMed]
- Wintermark M, Uske A, Chalaron M, et al. Multislice computerized tomography angiography in the evaluation of intracranial aneurysms: a comparison with intraarterial digital subtraction angiography. J Neurosurg 2003;98:828-36. [Crossref] [PubMed]
- Westerlaan HE, Gravendeel J, Fiore D, et al. Multislice CT angiography in the selection of patients with ruptured intracranial aneurysms suitable for clipping or coiling. Neuroradiology 2007;49:997-1007. [Crossref] [PubMed]
- Philipp LR, McCracken DJ, McCracken CE, et al. Comparison Between CTA and Digital Subtraction Angiography in the Diagnosis of Ruptured Aneurysms. Neurosurgery 2017;80:769-77. [Crossref] [PubMed]
- Menke J, Larsen J, Kallenberg K. Diagnosing cerebral aneurysms by computed tomographic angiography: meta-analysis. Ann Neurol 2011;69:646-54. [Crossref] [PubMed]
- Olin JW, Gornik HL, Bacharach JM, et al. Fibromuscular dysplasia: state of the science and critical unanswered questions: a scientific statement from the American Heart Association. Circulation 2014;129:1048-78. [Crossref] [PubMed]
Cite this article as: Hwa PC, Chiu YH, Liu LR, Chang WH. A case of spontaneous subarachnoid hemorrhage and intraventricular hemorrhage with negative computed tomography angiography findings. Health Technol 2019;3:10.